Cancer has ranked as the leading cause of death in Taiwan for many years. Cancers are generally named according to the organ from which the cancer cells originate. For example, cancer arising from lung cells is called lung cancer, cancer arising from liver cells is called liver cancer, and cancer arising from blood cells is called leukemia. One shared feature among Taiwan’s ten leading fatal cancers is that these cancer cells mainly originate from lesions in epithelial cells found in different organs.
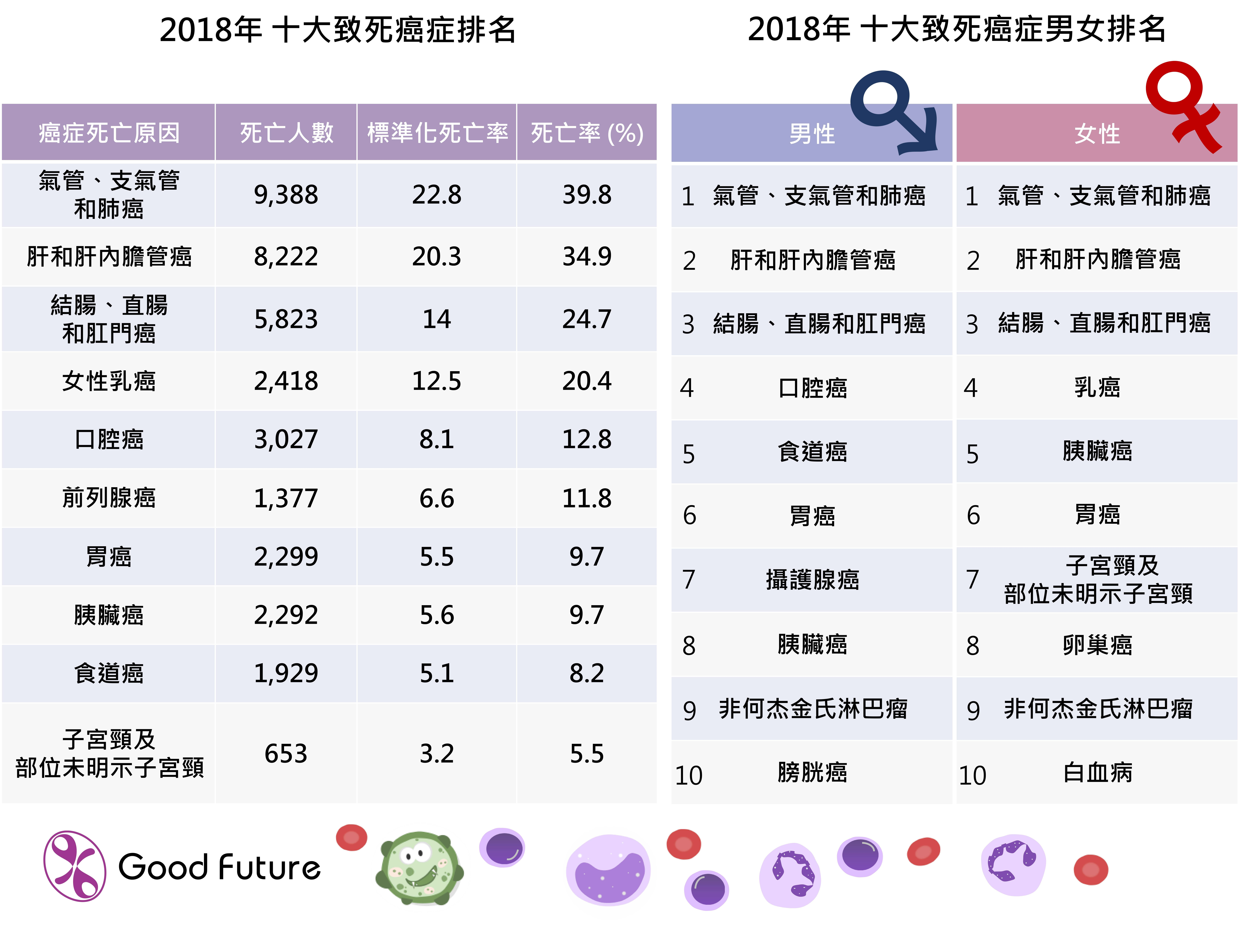
Figure 1. Ranking of the ten leading causes of cancer death in Taiwan. Source: Ministry of Health and Welfare, 2018 mortality statistics.
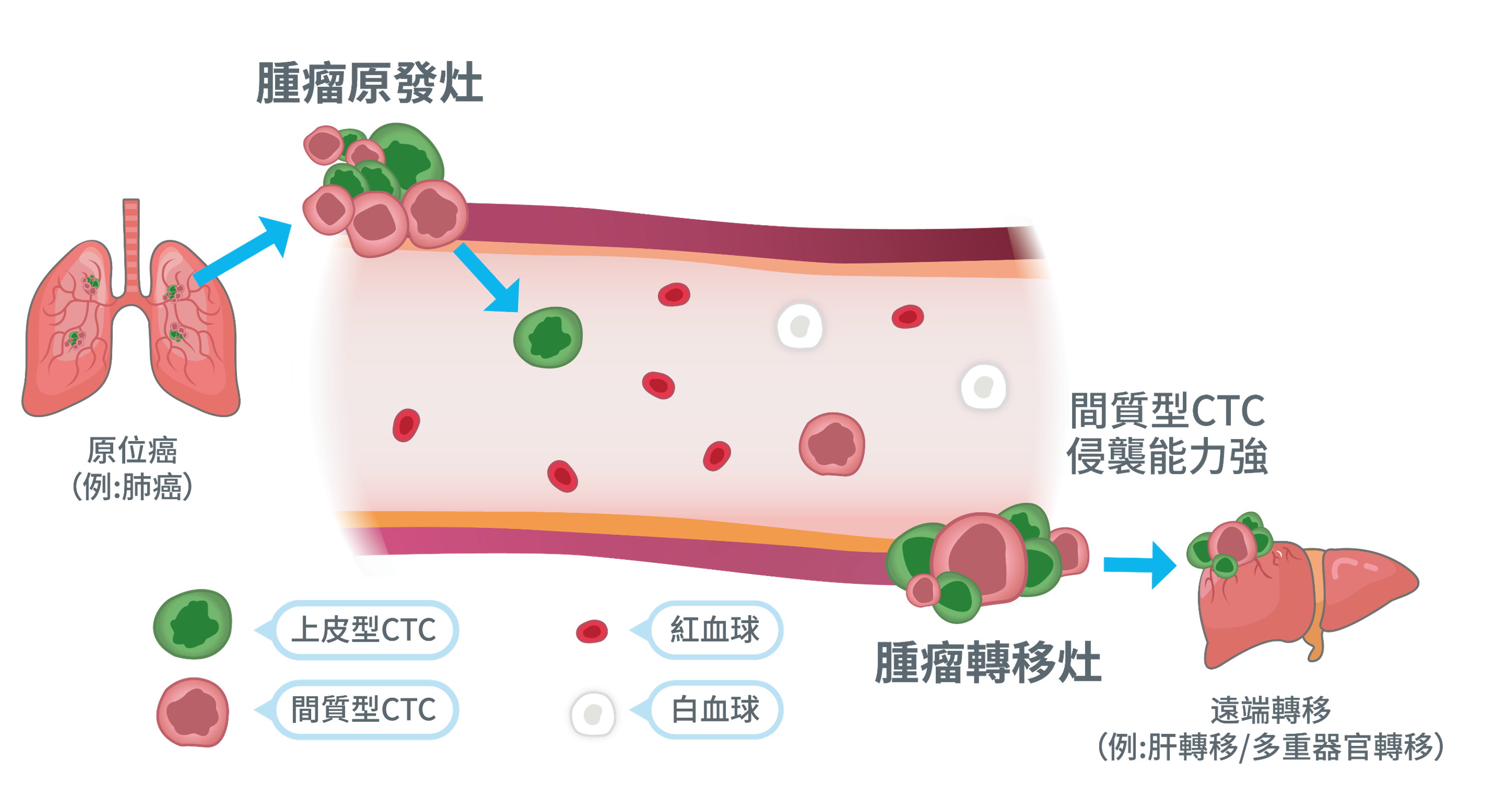
Cancer is so dangerous because cancer cells derived from epithelial lesions can spread to other organs, impair bodily function, and ultimately cause death. Medical research has confirmed that as long as cancer cells are present in the body, metastasis can occur. Every gram of cancer tissue can release about one million fresh cancer cells into nearby blood vessels each day, and these cells then circulate throughout the body in the bloodstream. These cancer cells that enter the blood are called circulating tumor cells (CTCs). Some of these cells may later invade tissues and continue proliferating, leading to metastasis. By the time cancer is detected, metastasis has often already begun. Even if the original tumor site is treated successfully, cancer cells that have already spread may continue dividing and accumulating, resulting in recurrence, which remains a major challenge for both patients and physicians.
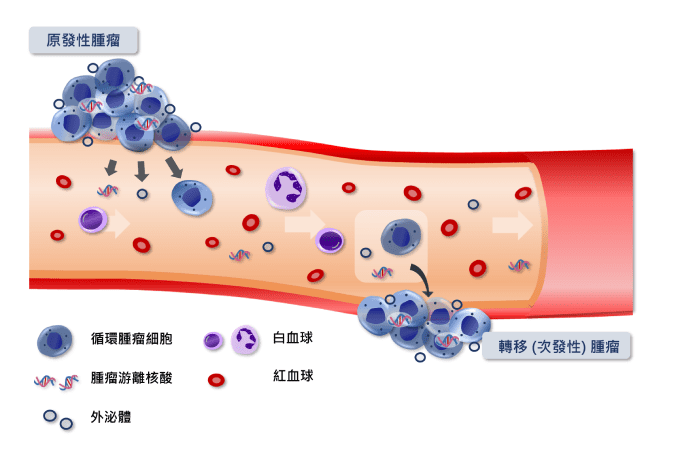
Figure 2. The process of cancer metastasis to distant organs. Cancer cells detach from the primary tumor, penetrate the vessel wall, enter the bloodstream as circulating tumor cells, and may later cross the vessel wall again to establish distant metastases. During this process, cancer cells also release cell-free nucleic acids and exosomes. These detectable cellular or molecular components in blood are collectively referred to as liquid biopsy materials.
If cancer cells can be detected before metastasis occurs, physicians may be able to remove localized lesions surgically and reduce the chance of metastasis and recurrence. Understanding how many cancer cells remain in the body can also help monitor treatment response and recurrence risk. Technologies that can detect whether cancer cells are present are therefore especially important. Imaging methods such as MRI and CT can identify tumors larger than 0.5 cm, but still have a certain margin of error, and very small lesions often require more sensitive testing methods for support. In recent years, liquid biopsy technologies have developed rapidly. In simple terms, liquid biopsy refers to using non-invasive blood testing to determine whether cancer cells (CTCs), cancer-derived nucleic acids (circulating tumor DNA or RNA), or exosomes are present in the blood, so as to better understand a subject’s condition. Each method has its own advantages, but detecting whether circulating tumor cells are present in blood can provide the most direct evidence because the cells themselves can be observed.
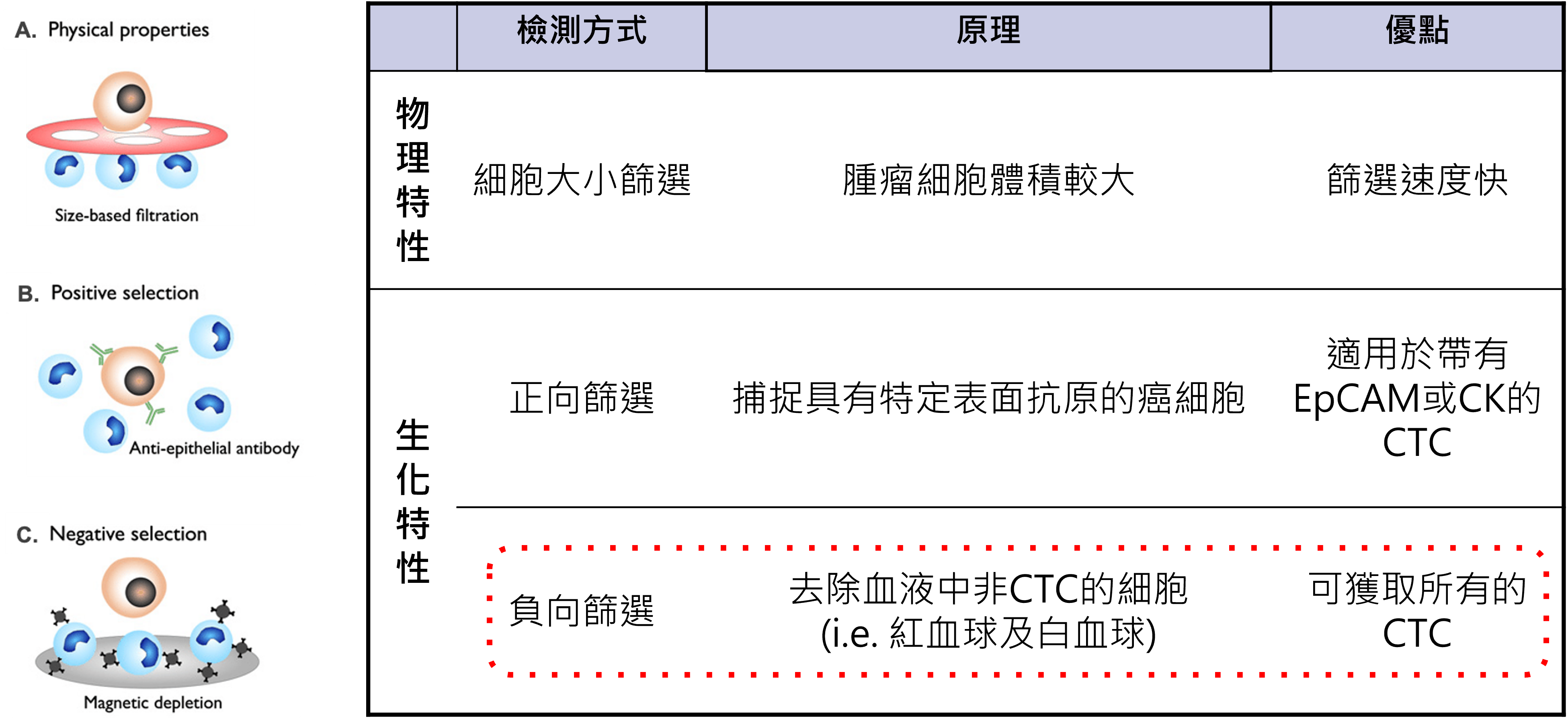
Circulating tumor cell testing is a technically demanding examination method. In practical terms, it involves enriching and immunofluorescently staining CTCs, acquiring fluorescent images, and identifying and counting the cells. There are several methods for CTC enrichment. Some rely on physical properties, such as differences in cell size or electric charge, to distinguish and enrich tumor cells. Because tumor cells are highly diverse, these methods may still miss certain cell populations and cannot comprehensively enrich all tumor cell types. Another approach uses biological properties to enrich CTCs. Methods that isolate cancer cells based on specific expressed proteins are called positive selection. However, this approach can only isolate CTCs that express the target marker and may still miss other relevant cells. In contrast, negative selection removes blood cells and preserves all non-blood cells. Comparatively, negative selection is more comprehensive in enriching different types of circulating tumor cells, making it better suited for downstream cellular and molecular analysis.
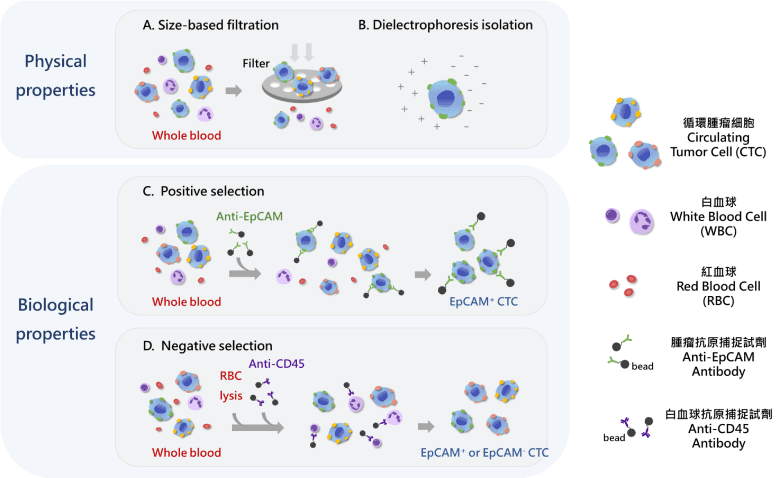
Figure 3. Principles of circulating tumor cell separation. Because circulating tumor cells and blood cells differ in physical characteristics, such as cell size and electrical properties, as well as biological characteristics, such as surface antigen expression, these differences can be used to develop different CTC enrichment methods.
Regardless of which method is used, circulating tumor cell testing is relatively convenient for the subject. Only a small amount of blood is needed, fasting is not required, and there is no need to worry about radiation exposure or contrast-agent allergy often associated with imaging tests. According to medical studies, when the number of circulating tumor cells in each milliliter of blood exceeds a certain range, there is a strong possibility that a cancer is developing in the body. The number of circulating tumor cells is also closely related to metastasis and treatment prognosis. Therefore, cancer patients, people with a family history of cancer, individuals with high-risk lifestyle factors such as smoking, alcohol consumption, high stress, frequent late nights, or long-term diets high in fat and low in vegetables and fruit, people suspected of having cancer, and even those undergoing regular health examinations may all benefit from circulating tumor cell testing. This can significantly improve cancer screening outcomes and the quality of treatment monitoring and disease management.